Can Sunlight Protect Your Kidneys From Sugar Damage?
Main Points
High blood sugar harms kidneys primarily by activating immune cells that release TNF-α, which then injures podocytes—the cells that maintain the kidney’s filtration barrier. Lower vitamin D status tracks with more TNF-α release under high-glucose conditions, implying that staying vitamin D–replete may help temper this inflammatory pathway. In clinical settings, activated vitamin D can improve some kidney markers and outcomes in people with established kidney disease, whereas standard vitamin D3 shows mixed, generally modest effects. Sunlight is useful for maintaining adequate vitamin D but is not a standalone kidney therapy. The most dependable actions remain controlling blood sugar, keeping blood pressure in range, and limiting kidney-toxic drugs; omega-3s may provide additional support in select cases.
Could sunlight—and more specifically, vitamin D made in your skin—help protect kidneys from damage caused by high blood sugar? There’s nuance here, but the short answer is “yes, potentially,” and in very specific ways. We’ll focus on a key kidney cell type, what high glucose does to those cells, and how vitamin D and sunlight fit into the picture.
Podocytes: The Kidney’s Gatekeepers
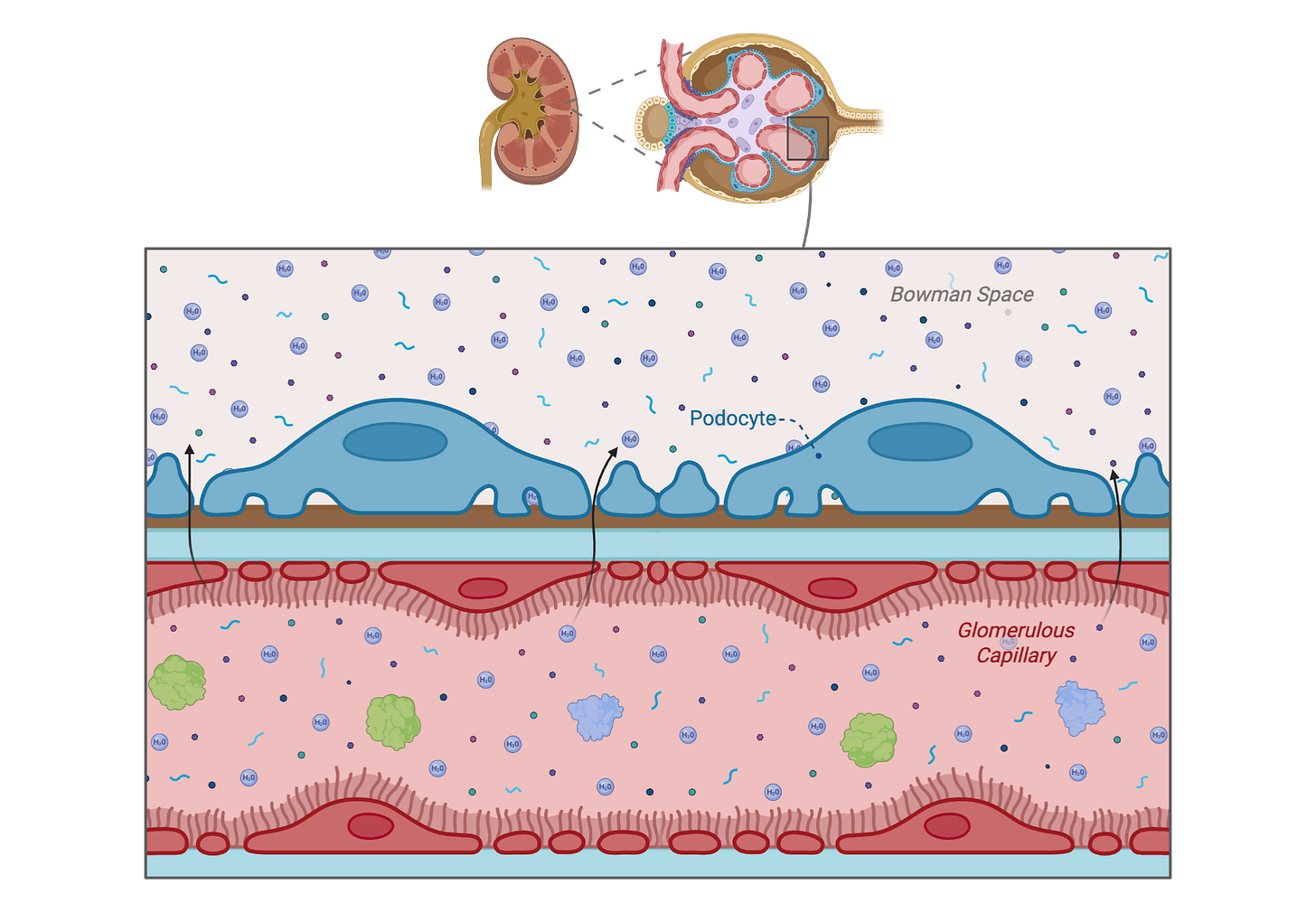
Podocytes wrap around the smallest blood vessels in the kidney’s filtering unit. Their interlocking “feet” form a selective barrier that lets water and small molecules pass into urine while keeping essential proteins like albumin in the bloodstream. If podocytes are injured, that barrier leaks, and protein shows up in urine—a warning sign your filter is failing.
High Blood Sugar: Direct vs Indirect Harm
Brief spikes of high glucose do not appear to directly injure podocytes by standard cell-death measures [523-524]. That raises a natural question: if glucose alone doesn’t immediately harm these cells, why does diabetes correlate with kidney decline?
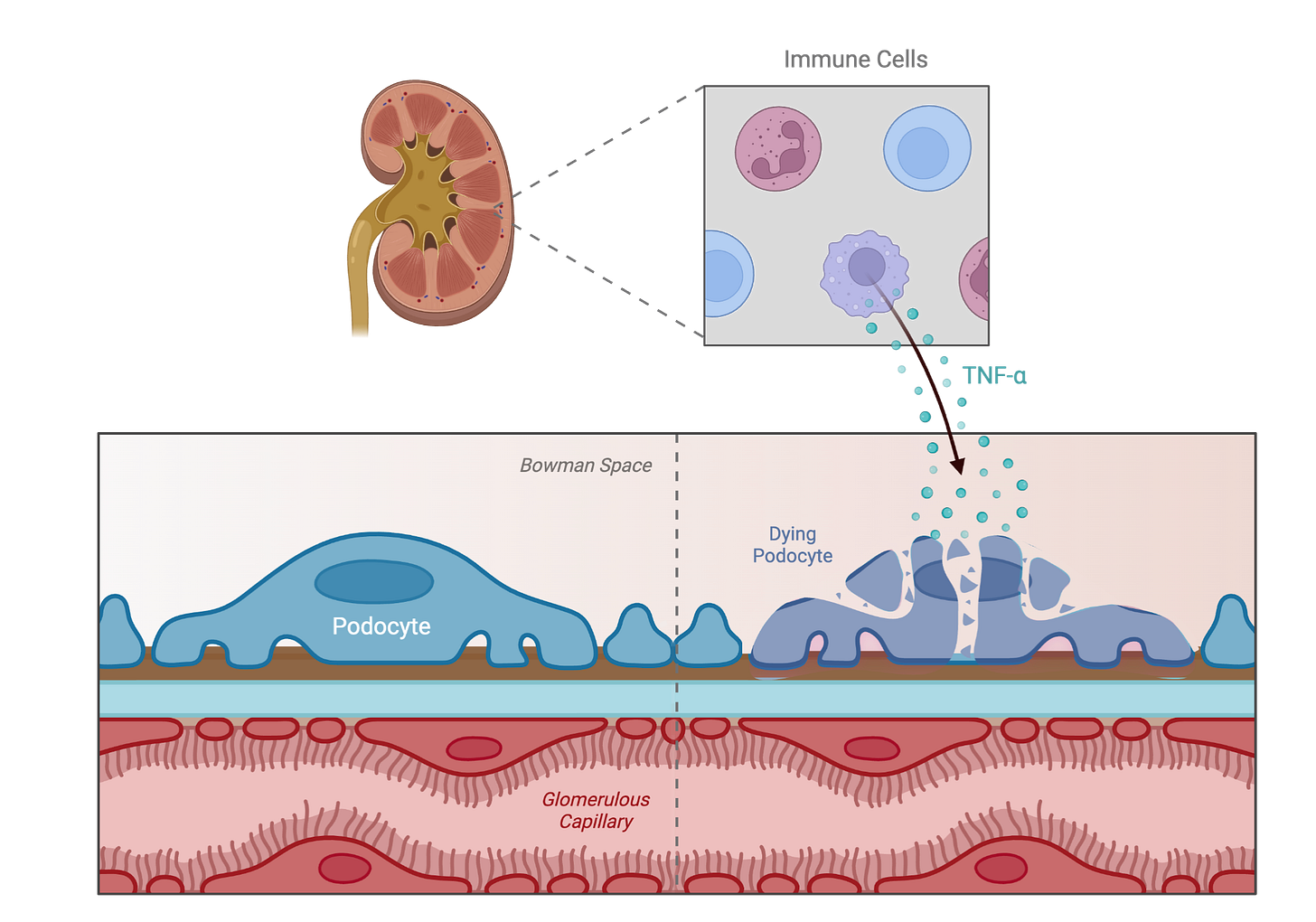
The answer, in this context, involves the immune system. When immune cells (particularly macrophages) are exposed to high glucose, they become more inflammatory. When those “primed” immune cells interact with podocytes, podocyte injury and cell-death signaling increase markedly. In other words, the damage is largely indirect: high glucose activates immune cells, and those cells then harm podocytes.
The Culprit Molecule: TNF-α
A central player here is tumor necrosis factor-alpha (TNF-α), a pro-inflammatory signal released by glucose-exposed immune cells. Elevated TNF-α in the kidney environment pushes podocytes toward dysfunction and death. Blocking TNF-α directly (for example, with antibodies in experimental settings) substantially protects podocytes, reinforcing that TNF-α is a key driver of injury.
Where Vitamin D Enters
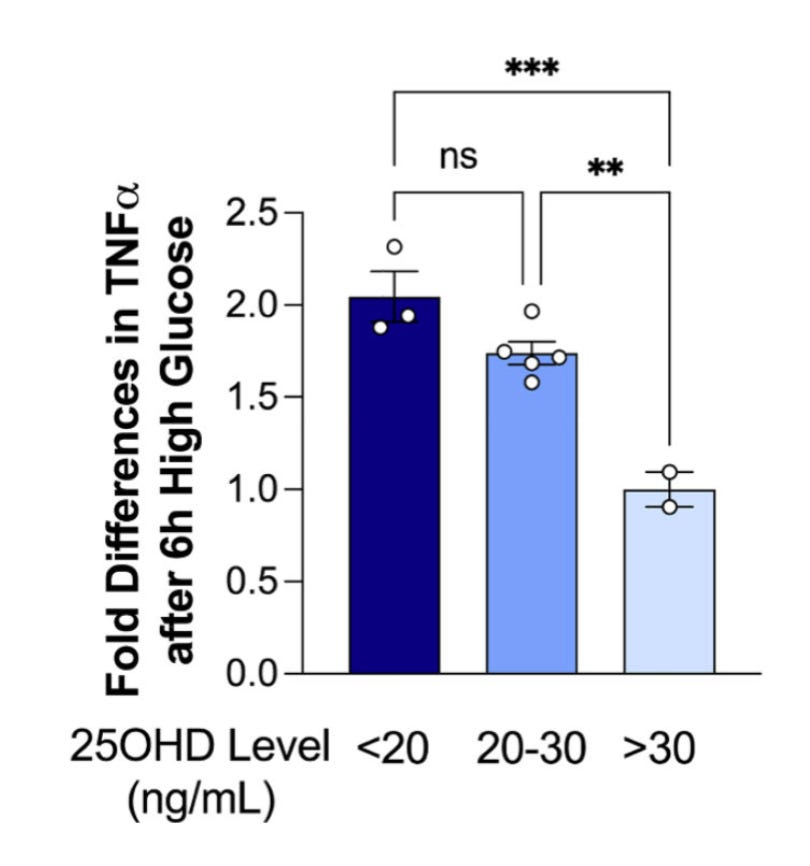
People with lower blood levels of vitamin D tend to show higher TNF-α release from their immune cells under high-glucose conditions (see figure below), whereas those with higher vitamin D levels show less. That pattern suggests vitamin D sufficiency may help keep immune over-activation—and thus TNF-α—more controlled, indirectly shielding podocytes from inflammatory damage.
More on the mechanisms:ADAM17 and TNF alpha
Other molecules indicated to reduce TNF alpha
All of that is included in the complete analysis, along with access to a private podcast, live sessions with me, a library of articles and videos, and much more as a Physionic Insider:
What Clinical Trials Suggest
Clinical research testing vitamin D for kidney outcomes is mixed and depends on context:
Activated forms of vitamin D (prescription medications) in people who already have chronic kidney disease [A] often improve markers like albumin in urine and are associated with reduced mortality in some studies.
Standard over-the-counter vitamin D3 shows mild or inconsistent effects on kidney function overall [B], and common global measures like estimated glomerular filtration rate (eGFR) frequently do not improve.
Taken together, correcting a deficiency is sensible, but routine supplementation beyond restoring normal levels hasn’t consistently translated into strong kidney benefits—unless you have diagnosed kidney disease and are using an activated form under medical supervision.
What About Sunlight?
Sunlight helps you make vitamin D, and maintaining a blood level in the normal range (for example, ≥30 ng/mL) is a reasonable target. Beyond maintaining adequacy, current evidence for sunlight exposure as a kidney-specific “treatment” is limited [C]. Casual, regular exposure that avoids sunburn is fine; just don’t expect sunlight alone to rescue kidney function.
More Direct Ways to Protect Your Kidneys
While nutrient strategies can help, the most reliable kidney-protective steps are:
Keep blood sugar in a healthy range
Maintain normal blood pressure
Avoid overusing nephrotoxic medications (for example, frequent use of certain over-the-counter pain relievers)
These interventions repeatedly show clear, practical benefits for preserving kidney function.
Main Points
High blood sugar harms kidneys primarily by activating immune cells that release TNF-α, which then injures podocytes—the cells that maintain the kidney’s filtration barrier. Lower vitamin D status tracks with more TNF-α release under high-glucose conditions, implying that staying vitamin D–replete may help temper this inflammatory pathway. In clinical settings, activated vitamin D can improve some kidney markers and outcomes in people with established kidney disease, whereas standard vitamin D3 shows mixed, generally modest effects. Sunlight is useful for maintaining adequate vitamin D but is not a standalone kidney therapy. The most dependable actions remain controlling blood sugar, keeping blood pressure in range, and limiting kidney-toxic drugs; omega-3s may provide additional support in select cases.
More on the mechanisms:ADAM17 and TNF alpha
Other molecules indicated to reduce TNF alpha
All of that is included in the complete analysis, along with access to a private podcast, live sessions with me, a library of articles and videos, and much more as a Physionic Insider:
Dr. Nicolas Verhoeven, PhD / Physionic
References
[Study 523] Zhang RM, Oh J, Wice BM, Dusso A, Bernal-Mizrachi C. Acute hyperglycemia induces podocyte apoptosis by monocyte TNF-α release, a process attenuated by vitamin D and GLP-1 receptor agonists. J Steroid Biochem Mol Biol. 2025;247:106676. doi:10.1016/j.jsbmb.2025.106676.
Funding/Conflicts: Mixed Funding [Public Funding: Supported by the National Institutes of Health/National Heart, Lung, and Blood Institute (R01HL09481806) and the U.S. Department of Veterans Affairs, VA Merit Award (I01BX003648). / Non-Profit Funding: American Heart Association Career Development Award (855967). // No direct Conflicts of Interest
[Study 524] Guo Y, Song Z, Zhou M, Yang Y, Zhao Y, Liu B, et al. Infiltrating macrophages in diabetic nephropathy promote podocytes apoptosis via TNF-α–ROS–p38 MAPK pathway. Oncotarget. 2017;8(32):53276-53287.
Funding/Conflicts: Public Funding [National Natural Science Foundation of China (No. 81370826; No. 81570612); Medical Key Talents Programs of Jiangsu Province (RC2011124); Clinical Medical Science Technology Special Project of Jiangsu Province (No. BL2014080); Fundamental Research Funds for the Central Universities of China; Jiangsu Province Ordinary University Graduate Research Innovation Project (KYLX15_0180).] // No direct Conflicts of Interest
[A] Kovesdy CP, Ahmadzadeh S, Anderson JE, Kalantar-Zadeh K. Association of activated vitamin D treatment and mortality in chronic kidney disease. Arch Intern Med. 2008;168(4):397-403. doi:10.1001/archinternmed.2007.110
[B] Wang Y, Yang S, Zhou Q, Zhang H, Yi B. Effects of Vitamin D Supplementation on Renal Function, Inflammation and Glycemic Control in Patients with Diabetic Nephropathy: a Systematic Review and Meta-Analysis. Kidney Blood Press Res. 2019;44(1):72-87. doi:10.1159/000498838
[C] Weller RB, Macintyre IM, Melville V, Farrugia M, Feelisch M, Webb DJ. The effect of daily UVA phototherapy for 2 weeks on clinic and 24-h blood pressure in individuals with mild hypertension. J Hum Hypertens. 2023;37(7):548-553. doi:10.1038/s41371-022-00729-2