One Sugar Creates a Unique Liver Harm, New Study
Main Points
Fructose appears capable of harming the liver not only through ordinary metabolic stress, but also through a microbiome-dependent pathway in which gut microbes convert fructose into acetaldehyde, a toxic compound also involved in alcohol metabolism. The strongest evidence suggests this is most relevant in the context of a poor, calorie-rich diet rather than fructose in isolation, which makes overall diet quality central to the problem. Reducing sugar-heavy, highly processed foods remains sensible, but increasing dietary fiber may be just as important because fiber may help prevent fructose from reaching the lower intestine, where microbes can convert it into harmful compounds. The clearest practical takeaway is to focus less on isolated fear of fructose alone and more on building a higher-fiber, less processed dietary pattern that protects the liver from the broader conditions in which this damage seems to occur.
Last year, research drew attention to the harm fructose can cause the liver. Newer findings [716] now add another strange and important layer to that story. Fructose appears capable of harming the liver in a way that resembles alcohol, not because it turns into alcohol itself, but because it can lead to the production of a toxic molecule that is closely associated with alcohol-related liver damage. There is also a practical angle here, because the same evidence points toward a relatively simple way to reduce some of that harm.
Fructose and Liver Disease Risk
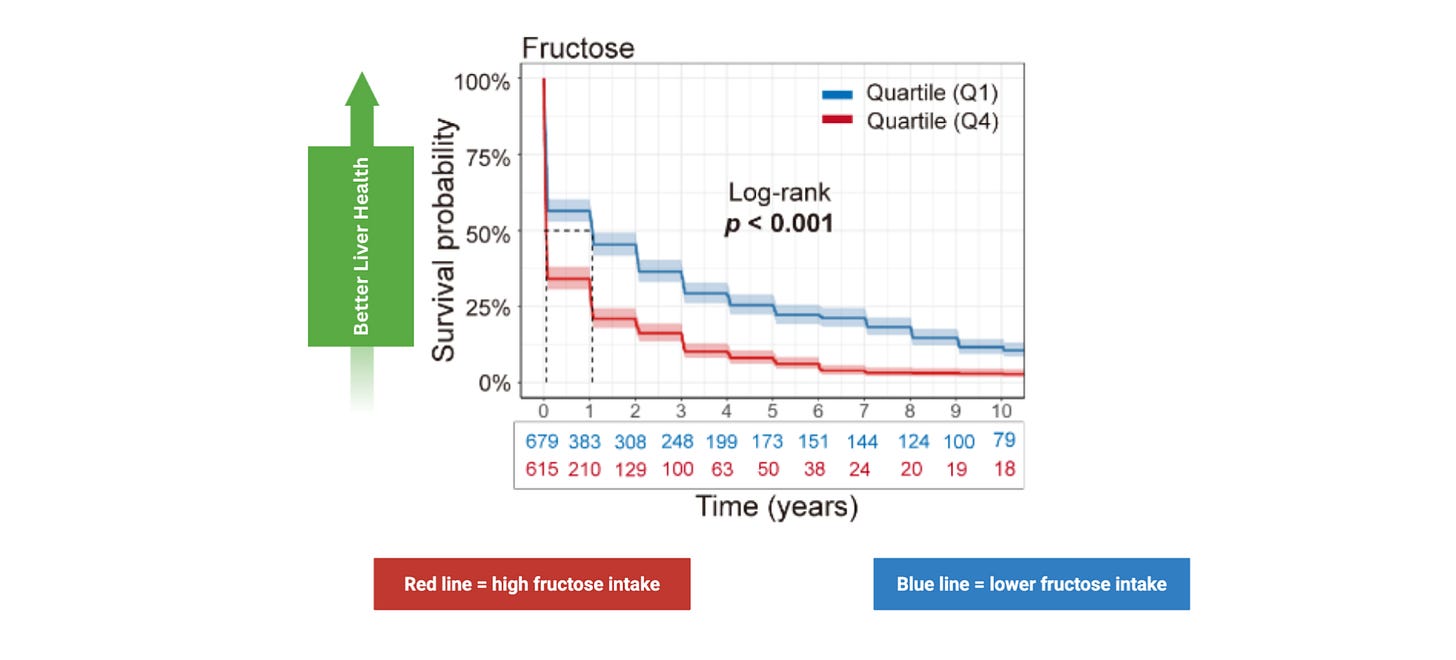
One of the opening findings is that higher fructose intake is associated with a greater projected probability of developing liver disease. Put simply, people consuming more fructose appear more likely to experience worse liver outcomes than people consuming less.
This kind of evidence is associative, which means it shows a relationship but does not by itself prove causation. Still, it gives an important starting point: higher fructose intake tracks with poorer liver health.
Technically, some of these data involve sugar intake as a whole, but fructose is often singled out as the most concerning component. Ordinary table sugar is made of two parts: glucose and fructose. While both affect metabolism, fructose is often viewed as the more problematic half when liver health is involved.
Direct Evidence from Experimental Models
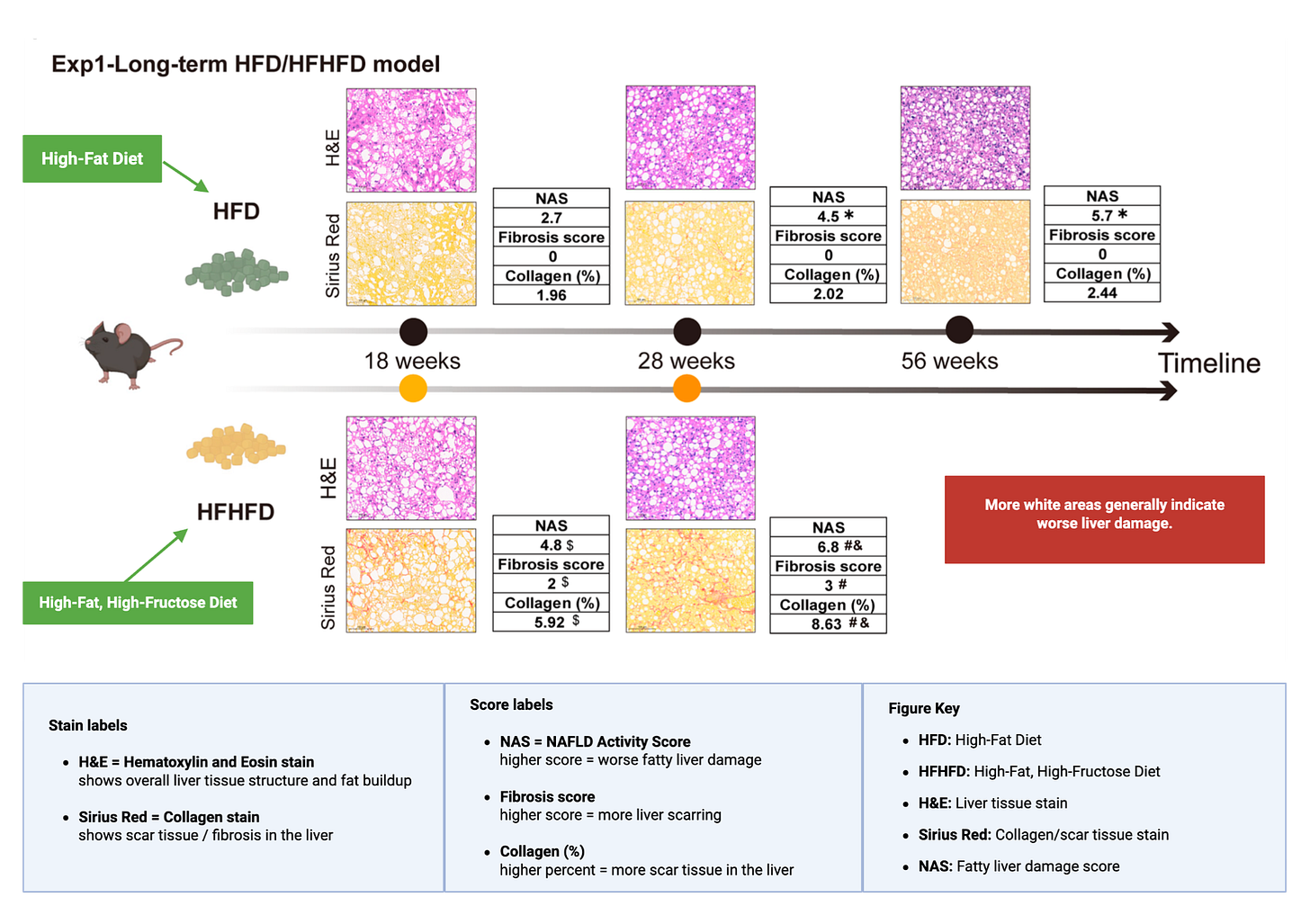
To get closer to showing a causal role, researchers also used direct experiments. Animals were fed either a control diet or a fructose-heavy diet, and liver tissue was then examined for fat accumulation and fibrosis. Fibrosis means scarring of tissue, and in the liver, it is a sign of worsening structural damage.
The results were clear. The fructose-heavy diet accelerated liver stress and damage. By 18 weeks, the animals eating high fructose had worse liver damage scores than the controls, and they reached that level much faster. In fact, the control condition only reached a similar degree of damage much later. In this setting, fructose was not simply associated with liver harm. It appeared to actively speed it up.
The Gut Microbiome Changes the Story
The story takes a surprising turn when the gut microbiome enters the picture. The gut microbiome is the enormous community of microbes living in the digestive tract. These organisms influence digestion, metabolism, immune function, and many other aspects of health.
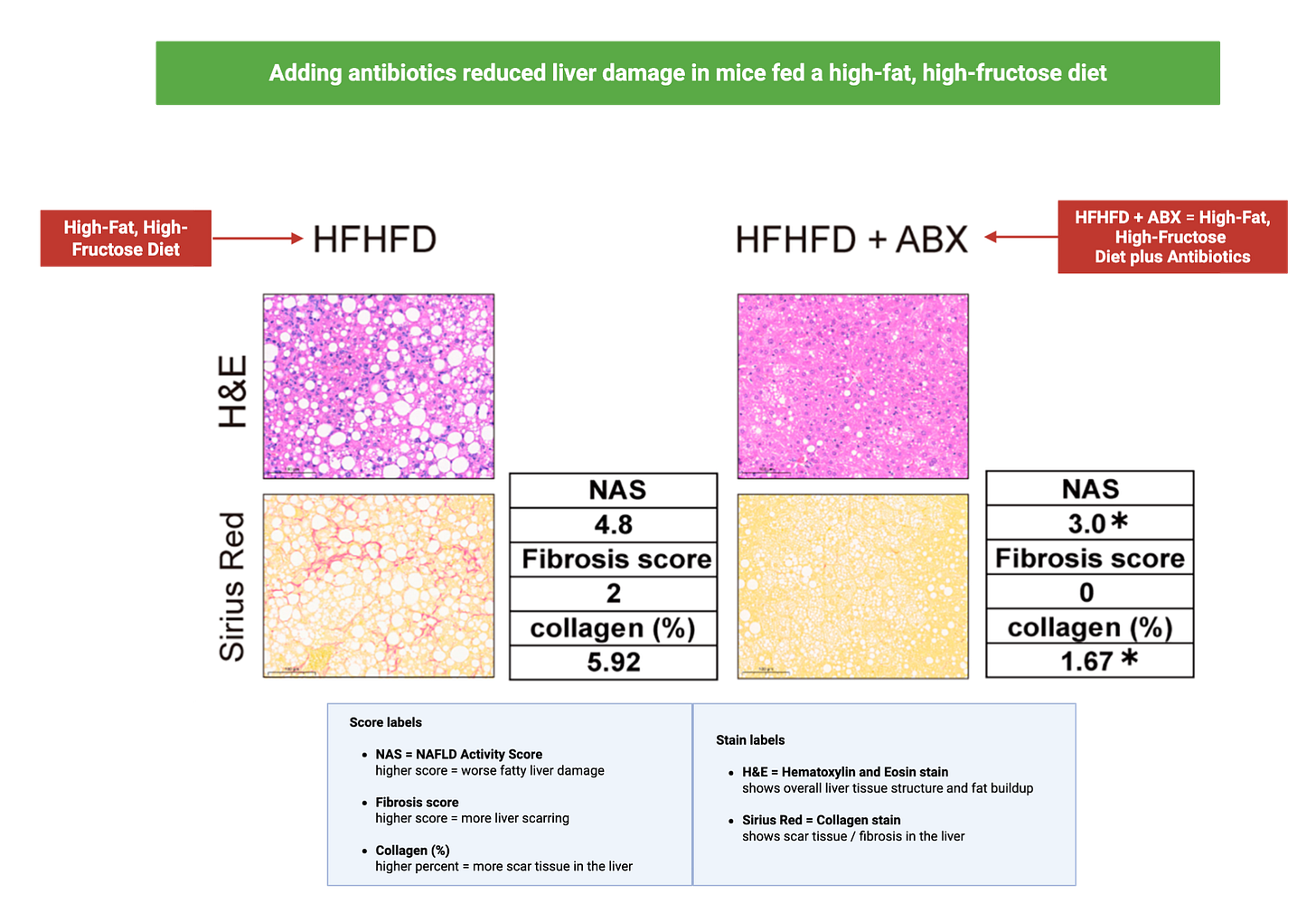
In the same fructose-heavy setting, researchers found that when animals were also given antibiotics to largely eliminate the microbiome, liver health improved. That is a striking result. It suggests that part of the harm was not coming from fructose alone, but from what gut microbes were doing with it.
This importantly changes the interpretation. Fructose may not only stress the liver directly. It may also create conditions in the gut that allow microbes to generate something harmful, which then affects the liver.
The Toxic Molecule: Acetaldehyde
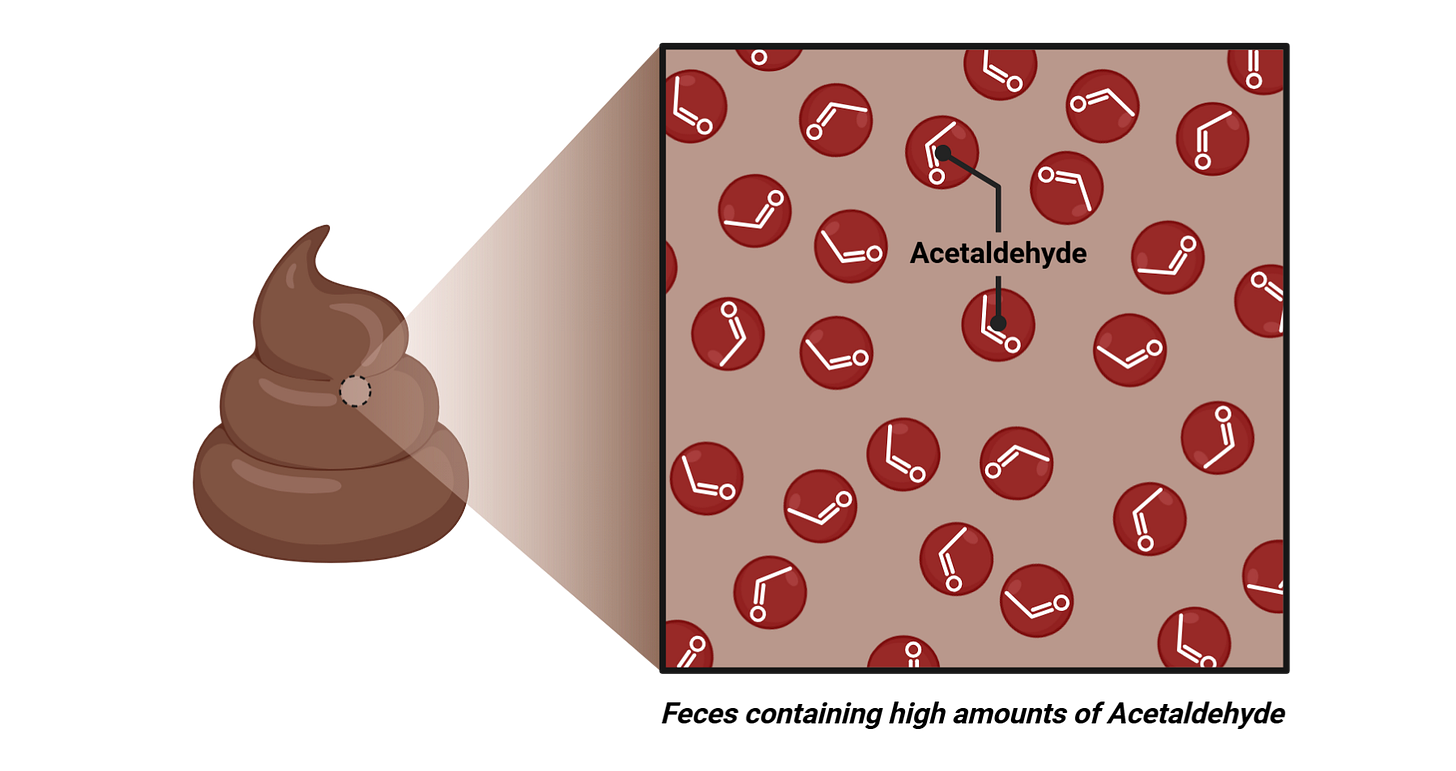
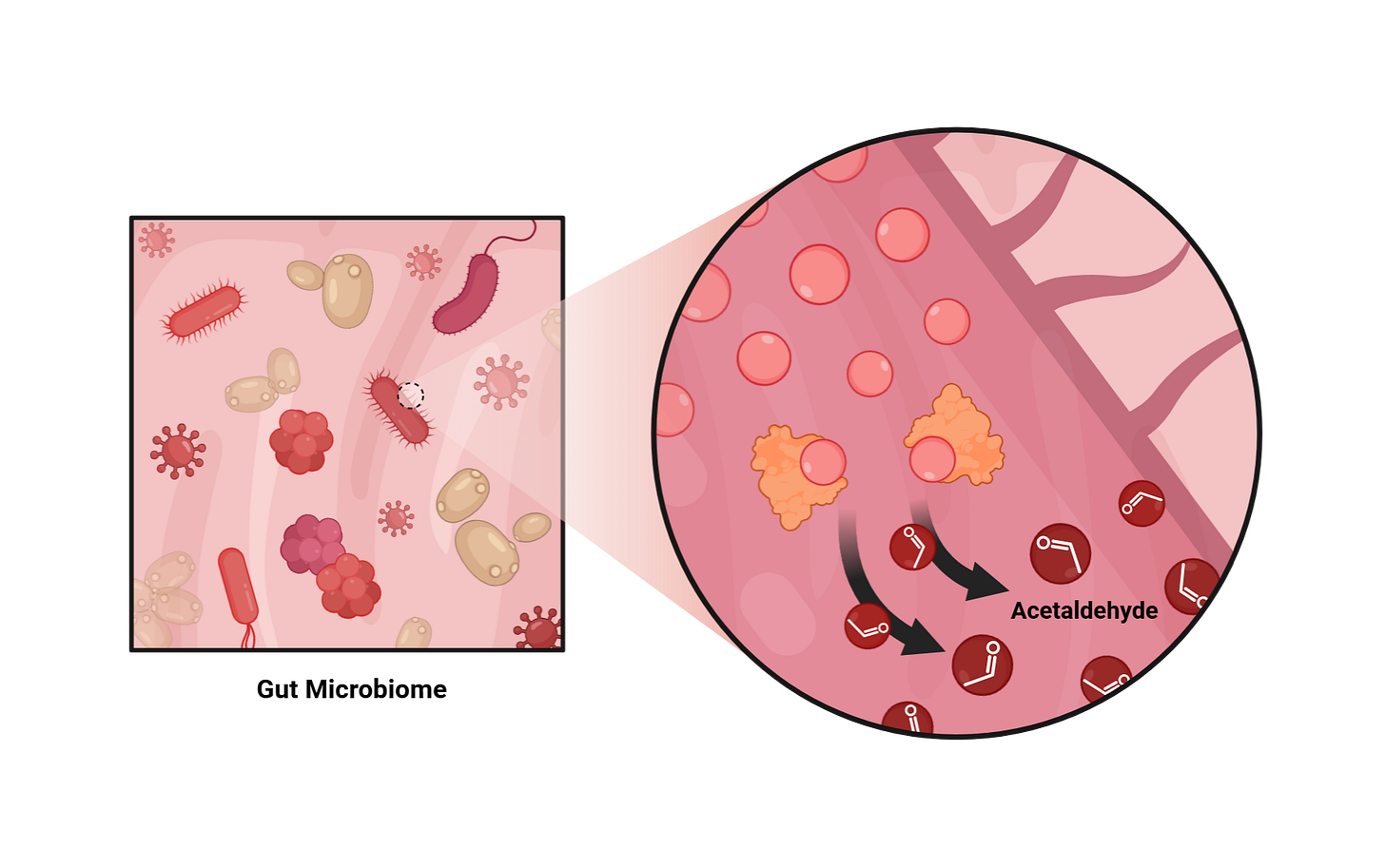
When researchers examined stool samples from people consuming fructose, one molecule stood out as being highly enriched: acetaldehyde.
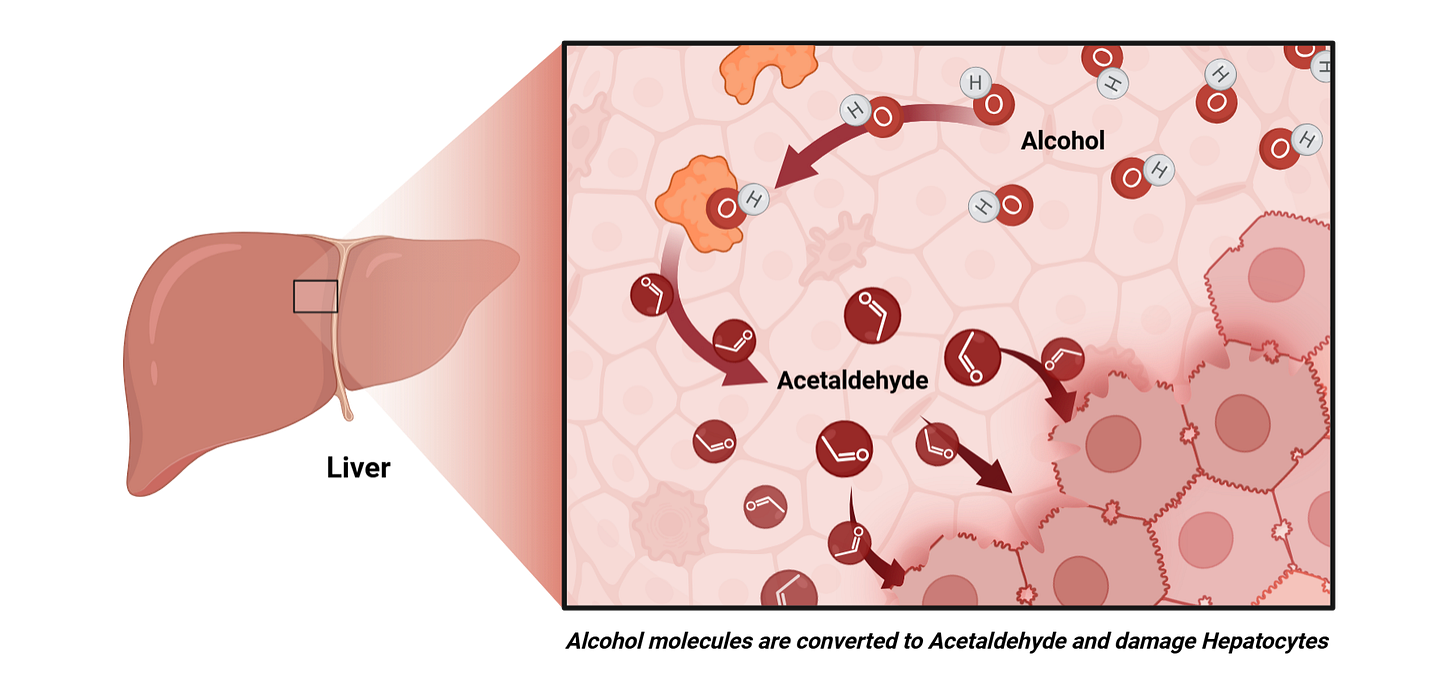
Acetaldehyde is a toxic intermediate, meaning it is a harmful molecule created during metabolism. Many people may not recognize the name at first, but it is the same molecule that alcohol is converted into in the liver. That is what makes it so relevant here. Acetaldehyde is well known for being toxic, and it is strongly linked to alcohol-related tissue damage.
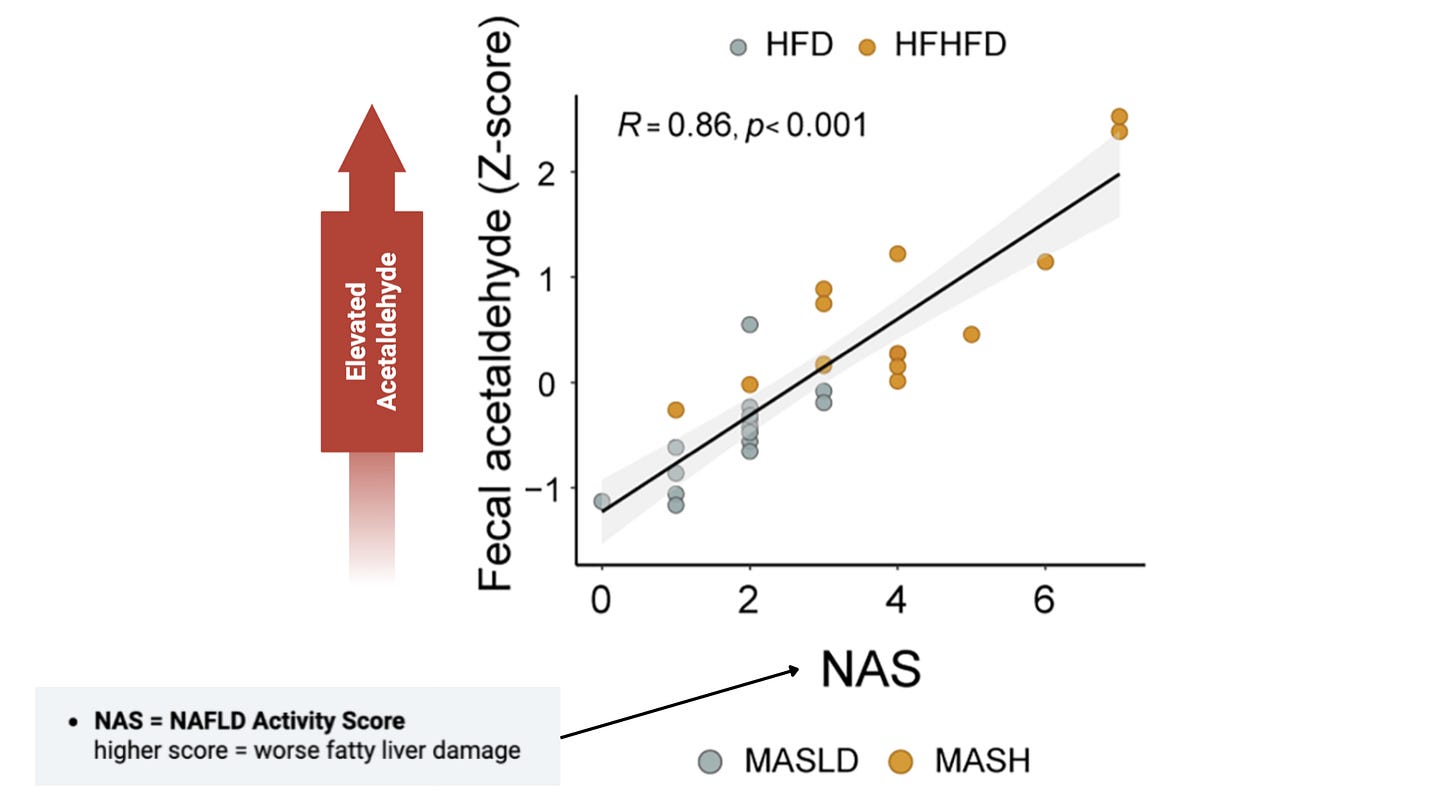
Researchers also found that higher acetaldehyde levels were associated with worse liver health. As acetaldehyde increased, liver markers worsened. That strengthens the case that acetaldehyde is not just present, but is likely part of the damaging process itself.
How Fructose Leads to Acetaldehyde
The obvious question is where this acetaldehyde is coming from if no alcohol is being consumed.
The proposed answer is the gut microbiome. Certain microbes appear to have enzymes that can convert fructose into metabolic intermediates, such as pyruvate, which can then be converted into acetaldehyde.
In simple terms, some gut microbes seem able to process fructose in a way that produces this toxic byproduct.
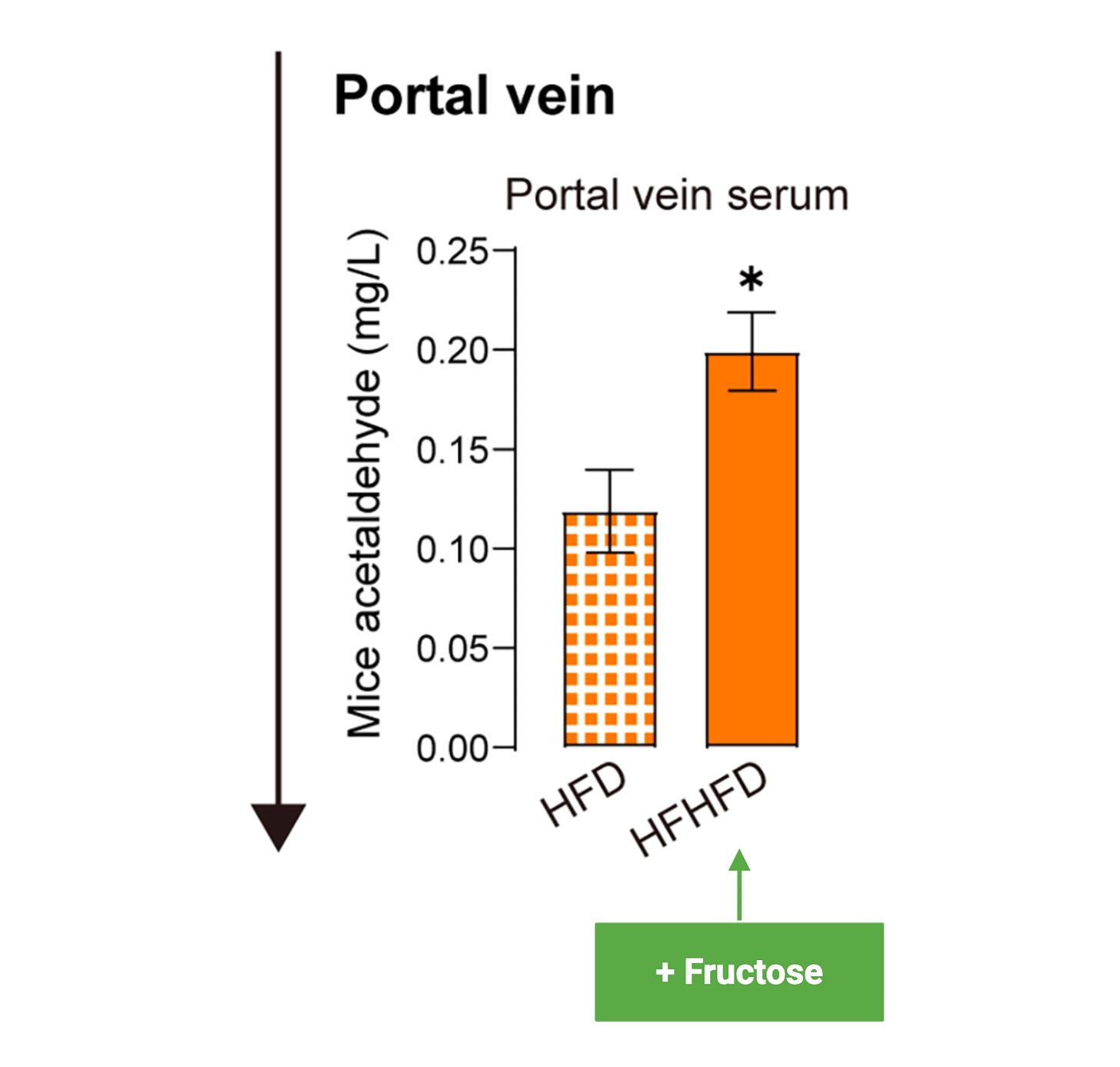
Researchers supported this by exposing gut microbes and human stool samples to fructose and then measuring what was produced. Acetaldehyde levels increased. So the basic chain appears to be this: fructose reaches the gut, microbes act on it, acetaldehyde is generated, and that acetaldehyde contributes to liver injury.
This is what makes the mechanism so fascinating. Through the microbiome, fructose may create an alcohol-related toxin without any alcohol being consumed at all.
Stellate Cells, MMP7, and Liver Damage
The achE enzyme and eliminating acetaldehyde
Assessing different Fiber Types and Doses on Liver Health
All of these topics are explored in depth in the complete analysis, along with access to a private podcast, live sessions, a growing research library, and practical breakdowns—available exclusively to Physionic Insiders.
Why Eliminating the Microbiome Is Not a Real Solution
Even though removing much of the microbiome improved liver measures in the experiment, that is obviously not a realistic strategy in everyday life. The microbiome is essential to health overall, and destroying it would create many other problems.
So the real question is not whether the microbiome matters. It clearly does. The practical question is how to alter the microbiome in a way that reduces harmful activity without wiping the whole system out.
Researchers did not stop at identifying the problem. They also explored whether the microbiome could be reshaped to help solve it through genetically engineered microbes delivered as a probiotic.
The Most Accessible Strategy: Reduce Fructose Exposure
Still, genetically engineered microbes are not a practical option for almost everyone. So the most obvious solution is to reduce fructose intake. That sounds simple, but it becomes more complicated in real life because fructose is everywhere. It is easy to identify in sugar-sweetened drinks and heavily processed foods, but it is also found in foods that are usually considered healthy, such as fruit.
That means not all fructose-containing foods should be treated as equal. The broader dietary context matters.
A Practical Alternative: Fiber
A more realistic and accessible strategy may be to focus on dietary fiber. Dietary fiber is the part of plant foods that the body does not fully digest. It influences how nutrients move through the digestive tract and can also reshape the microbiome.
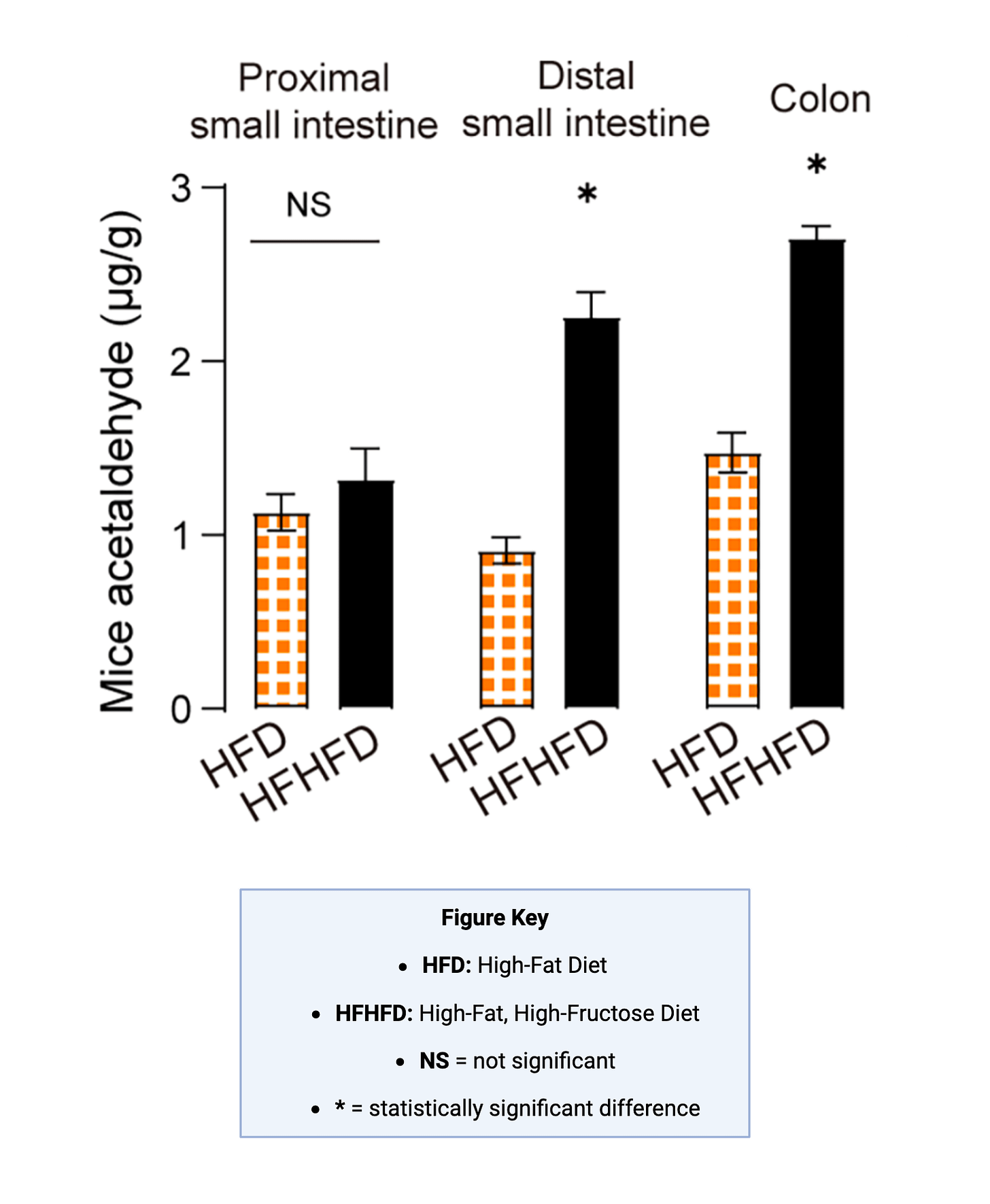
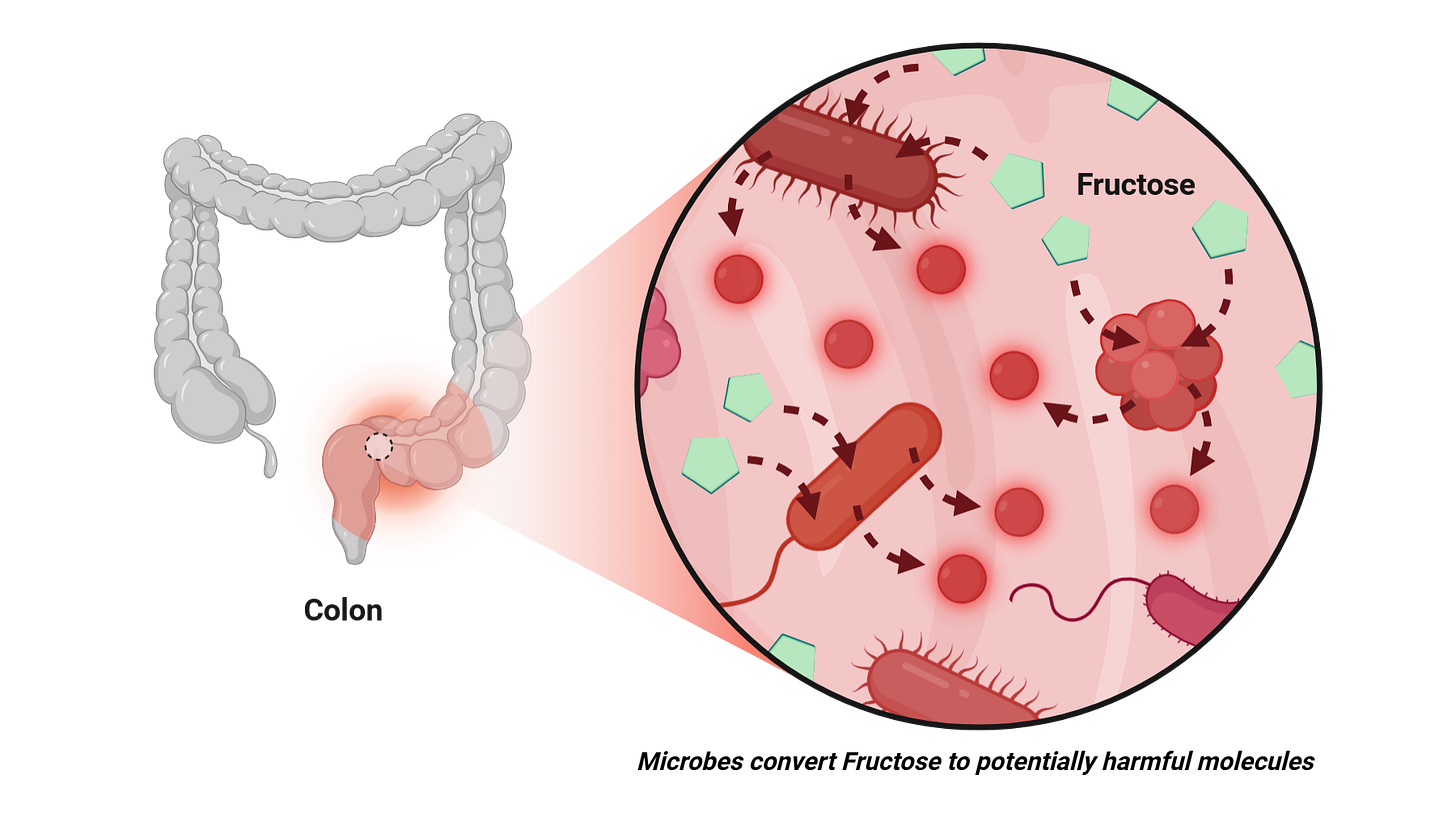
In the newer evidence, acetaldehyde production was especially elevated in the later portions of the small intestine and in the colon.
This connects well with a previously described ‘Fructose Spillover Effect’, in which fructose reaches the later stages of the intestine and is then converted by microbes into potentially harmful molecules.
In earlier work [535], dietary fiber prevented fructose from reaching those lower intestinal regions in the same way. If fructose does not reach those microbes, the microbes have less opportunity to convert it into harmful compounds. There is not yet direct proof that fiber lowers acetaldehyde production in this exact model, but the logic fits well.
Fiber also seems to help in two broader ways. First, it often shifts the microbiome in a more favorable direction. Second, it tends to improve liver health overall. Together, that makes fiber a strong, practical candidate for reducing this type of liver stress.
This may also help explain why whole foods like fruit do not show the same negative pattern as highly processed, sugar-heavy foods. In whole foods, fructose comes packaged with fiber and a different food structure, which likely changes how much fructose reaches the lower gut and how microbes respond.
Important Nuance and Limits
Even though this mechanism is compelling, there are important limits to keep in mind. The early data linking fructose with liver disease risk are associative, so they do not fully control for all the other factors that affect liver health.
The amount of fructose consumed in some of the evidence was also extremely high, around 150 grams or more, which roughly translates to about 300 grams of total sugar. That is far above what many people consume on a typical day, so it may not apply equally to everyone.
There is also a lack of long-term studies looking specifically at fructose intake and liver health. There are, however, some studies [1] on sugar-sweetened beverages, which are a major source of fructose. In those studies, higher consumption was associated with worse liver health even after adjusting for factors like body weight, physical activity, and overall diet. That suggests the broader concern is probably real, and notably, the associations appeared at much lower intakes than the extreme amounts discussed earlier.
At the same time, not all intervention studies agree. Some show no liver harm from fructose [2], while others do [3, 4]. Even in the main study discussed here, the animals were eating a calorie-rich diet and then consuming fructose on top of that. That likely matters a great deal.
The Bigger Picture
The most consistent interpretation is that fructose appears most harmful in the setting of a poor overall diet, especially one high in calories, highly processed foods, and likely to promote weight gain. In that setting, the mechanisms described here, including microbiome-driven acetaldehyde production, are likely very relevant.
When fructose is studied in tighter, more controlled settings and removed from that broader, unhealthy dietary pattern, the evidence becomes less consistent. That does not mean fructose is harmless. It means the context in which it is consumed likely determines how harmful it becomes.
So the most reasonable conclusion is not that all fructose should be feared equally. It is that fructose becomes more problematic when it is part of a broader diet that is already pushing the liver toward fat accumulation and stress. In that setting, the microbiome may amplify the problem by generating acetaldehyde.
Why This Mechanism Matters
Even with the remaining uncertainty, this new mechanism is remarkable. The idea that sugar can interact with gut microbes to produce an alcohol-related toxin offers a deeper explanation for how diet, the microbiome, and liver health intersect.
It also offers a practical direction. Improving diet quality and maintaining regular fiber intake may reduce the chance that fructose reaches the parts of the gut where it can be converted into harmful compounds. That is a far more realistic strategy for most people than trying to manipulate the microbiome with engineered microbes.
Main Points
Fructose appears capable of harming the liver not only through ordinary metabolic stress, but also through a microbiome-dependent pathway in which gut microbes convert fructose into acetaldehyde, a toxic compound also involved in alcohol metabolism. The strongest evidence suggests this is most relevant in the context of a poor, calorie-rich diet rather than fructose in isolation, which makes overall diet quality central to the problem. Reducing sugar-heavy, highly processed foods remains sensible, but increasing dietary fiber may be just as important because fiber may help prevent fructose from reaching the lower intestine, where microbes can convert it into harmful compounds. The clearest practical takeaway is to focus less on isolated fear of fructose alone and more on building a higher-fiber, less processed dietary pattern that protects the liver from the broader conditions in which this damage seems to occur.
Stellate Cells, MMP7, and Liver Damage
The achE enzyme and eliminating acetaldehyde
Assessing different Fiber Types and Doses on Liver Health
All of these topics are explored in depth in the complete analysis, along with access to a private podcast, live sessions, a growing research library, and practical breakdowns—available exclusively to Physionic Insiders.
Dr. Nicolas Verhoeven, PhD / Physionic
References
[Study 716] Tang Y, Kuang J, Xia X, et al. Targeting microbiota-generated acetaldehyde to prevent progression of metabolic dysfunction-associated steatotic liver disease. Cell Metab. 2026;38:1-15. doi:10.1016/j.cmet.2026.01.021
Funding/Conflict: Public Funding: From the study, this work was supported by the Noncommunicable Chronic Diseases–National Science and Technology Major Project (2023ZD0507600 and 2025ZD0551000) and the National Natural Science Foundation of China; Non-Profit Funding: From the study, I did not find non-profit funding reported; Industry Funding: From the study, I did not find industry funding reported; Conflicts of Interest: From the study, the authors declared no competing interests.
[Study 535] Jung S, Bae H, Song WS, et al. Dietary fibre-adapted gut microbiome clears dietary fructose and reverses hepatic steatosis. Nat Metab. 2025;7(9):1801-1818. doi:10.1038/s42255-025-01356-0.
[Study 606] Ni Y, Qian L, Leal Siliceo S, et al. Resistant starch decreases intrahepatic triglycerides in patients with NAFLD via gut microbiome alterations. Cell Metab. 2023;35(9):1530-1547. doi:10.1016/j.cmet.2023.08.002
Funding/Conflict: Public Funding: From the study, support was reported from the National Research Foundation of Korea, the Ministry of Health & Welfare of the Republic of Korea, and the National Institutes of Health/National Cancer Institute, including grants R01-AA029124, R21-AA030358, T32GM008620, F31DK134173, K22-CA234399, P30CA062203, R01CA244519, and R01CA259370; Non-Profit Funding: From the study, support was also reported from the American Diabetes Association, the AASLD Foundation Pinnacle Research Award in Liver Disease, the Edward Mallinckrodt, Jr. Foundation Award, the Pew Foundation, and the V Foundation for Cancer Research; Industry Funding: From the study, Johnson & Johnson supported S.M.; Conflicts of Interest: From the study, the authors declared no competing interests.
[1] Park WY, Yiannakou I, Petersen JM, Hoffmann U, Ma J, Long MT. Sugar-Sweetened Beverage, Diet Soda, and Nonalcoholic Fatty Liver Disease Over 6 Years: The Framingham Heart Study. Clin Gastroenterol Hepatol. 2022;20(11):2524-2532.e2. doi:10.1016/j.cgh.2021.11.001
[2] Johnston RD, Stephenson MC, Crossland H, et al. No difference between high-fructose and high-glucose diets on liver triacylglycerol or biochemistry in healthy overweight men. Gastroenterology. 2013;145(5):1016-1025.e2.doi:10.1053/j.gastro.2013.07.012
[3] Maersk M, Belza A, Stødkilde-Jørgensen H, et al. Sucrose-sweetened beverages increase fat storage in the liver, muscle, and visceral fat depot: a 6-mo randomized intervention study. Am J Clin Nutr. 2012;95(2):283-289. doi:10.3945/ajcn.111.022533
[4] Schwarz JM, Noworolski SM, Wen MJ, et al. Effect of a High-Fructose Weight-Maintaining Diet on Lipogenesis and Liver Fat. J Clin Endocrinol Metab. 2015;100(6):2434-2442. doi:10.1210/jc.2014-3678
[5] Daubioul CA, Horsmans Y, Lambert P, Danse E, Delzenne NM. Effects of oligofructose on glucose and lipid metabolism in patients with nonalcoholic steatohepatitis: results of a pilot study. Eur J Clin Nutr. 2005;59(5):723-726. doi:10.1038/sj.ejcn.1602127
[Study 606] Ni Y, Qian L, Leal Siliceo S, et al. Resistant starch decreases intrahepatic triglycerides in patients with NAFLD via gut microbiome alterations. Cell Metab. 2023;35(9):1530-1547. doi:10.1016/j.cmet.2023.08.002
Funding/Conflict: Public Funding: From the study, support was reported from the National Natural Science Foundation of China, Shanghai Municipal Key Clinical Specialty, Shanghai Research Center for Endocrine and Metabolic Diseases, the National Key Research and Development Program of China, the Marie Sklodowska-Curie Actions and Innovative Training Networks, Shanghai Jiao Tong University School of Medicine, and the Dalian Institute of Chemical Physics, Chinese Academy of Sciences; Non-Profit Funding: From the study, additional support from the Key Foundation was listed, but I could not verify its exact funding type from the available source; Industry Funding: From the study, I did not find industry funding reported; Conflicts of Interest: From the study, the authors declared no competing interests.
[Study 608] Li H, Zhang L, Li J, et al. Resistant starch intake facilitates weight loss in humans by reshaping the gut microbiota. Nat Metab. 2024;6(3):578-597. doi:10.1038/s42255-024-00988-y
Funding/Conflict: Public Funding: From the study, support was reported from the National Key Research and Development Program of China (2022YFA1004804), Shanghai Municipal Key Clinical Specialty, Shanghai Research Center for Endocrine and Metabolic Diseases (2022ZZ01002), the National Natural Science Foundation of China, including major international joint research project 81220108006, Excellent Young Scientists Fund 82022012, General Fund 82270907, Major Program 92357305, the Innovative Research Team of High-level Local Universities in Shanghai (SHSMU-ZDCX20212700), the Hong Kong Scholars Program (XJ2013035), Shanghai Jiao Tong University School of Medicine Two Hundred Program, Hong Kong Research Grant Council (AOE/M/707-18), Marie Sklodowska-Curie Actions and Innovative Training Networks (H2020-MSCA-ITN-2018 813781), DFG under Germany’s Excellence Strategy (EXC 2051; project ID 390713860), Shenzhen Basic Research Program (JCYJ20190808182402941), Guangdong Basic and Applied Research Major Program (2019B030302005), the Key Foundation of NSFC (21934006), the Strategic Priority Research Program (B) of the Chinese Academy of Sciences (XDB38020200), the Youth Innovation Promotion Association of the Chinese Academy of Sciences (2021186), and The Hong Kong Polytechnic University (P0042740); Non-Profit Funding: From the study, no non-profit funding was reported; Industry Funding: From the study, no industry funding was reported; Conflicts of Interest: From the study, the authors declared no competing interests.