The Most Mind-Blowing Study on Fiber I’ve Ever Read
Main Points
Fiber has always had a good reputation, but this new work makes that reputation specific and mechanistic. In animals overloaded with fructose, adding inulin — a fermentable fiber — dramatically reduced fat buildup in the liver and improved liver structure. Inulin did this by (1) turning down the genes that turn sugar into fat and (2) encouraging the liver to burn fat instead of hoarding it. It also (3) blocked fructose spillover into the colon, preventing downstream gut damage and reducing the constant fat assault on the liver. Practically, that means inulin-rich foods like chicory root, Jerusalem artichokes, garlic, leeks, and onions are not just “fiber sources,” they are liver-protective tools. If you’re dealing with, or worried about, fatty liver, especially from fructose-heavy eating patterns, prioritizing those foods (or carefully using inulin supplements, if you tolerate them) is a direct, biological way to defend your liver. And while cutting sugary fructose-heavy drinks is smart, some of inulin’s benefits are independent of fructose restriction — so fiber isn’t just damage control, it’s active protection.
There are two ways I could start talking about fiber. I could go full “TV infomercial,” yelling about how unbelievably life-changing it is. Or I could go full calm-and-cozy, like Mister Rogers or Bob Ross: “Hey there, friend… what a beautiful day to chat about fiber.”
Either way, I want you to know two things right away. First, fiber has consistently been linked to better health across many human studies [A-E]. We’re talking improvements in heart health, blood pressure, blood sugar control, and digestion. When researchers look at large groups of people, those who eat more fiber tend to have lower risk of disease and tend to age better - simple as that.
Second, one of the main reasons fiber is believed to help so many parts of the body is that certain fibers get eaten by your gut microbes — the bacteria in your intestines — and are turned into short-chain fats (also called short-chain fatty acids, or SCFAs). These short-chain fats (like acetate, propionate, and butyrate) then act almost like messengers. They travel around the body and talk to different organs, calming inflammation, helping metabolism, and keeping tissues healthy.
All of that is true… but it’s also kind of boring because you’ve probably heard “fiber feeds gut bacteria and makes short-chain fats” before.
What I couldn’t have told you until recently is what I can tell you now, because of a new study [535]. And this is where things stop being boring.
Fructose, Fiber, and the Liver
Here’s what the researchers did - they made mice unhealthy by feeding them fructose. Fructose is a type of sugar. It’s found in table sugar (sucrose is half fructose), in high-fructose corn syrup, and in a lot of sweetened drinks. High fructose intake has been tied to fatty liver — basically, the liver starts creating and storing too much fat, which can lead to a condition often called “fatty liver disease.”
Now, they didn’t just feed some mice fructose. They also had another group of mice that got fructose plus a specific fiber called inulin. Inulin is a fermentable fiber, meaning your gut bacteria can eat it.
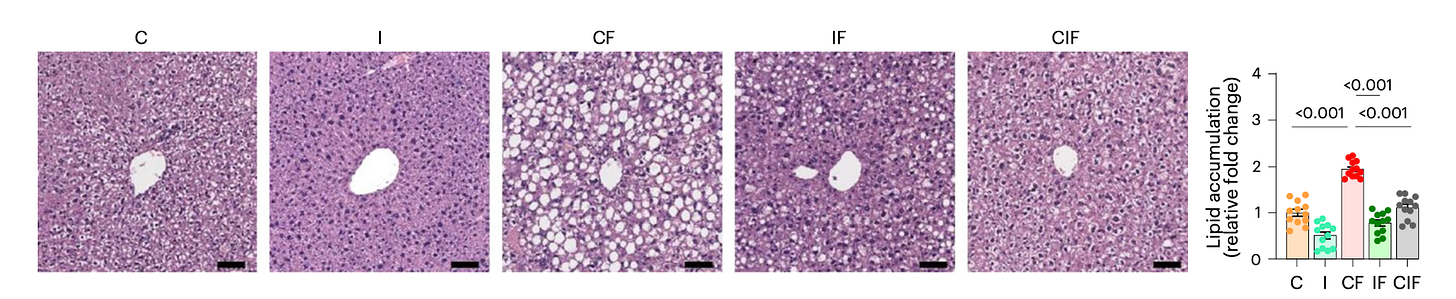
Then they compared the livers of these groups. When you look at liver tissue under a microscope, you can stain it so fat shows up as white. The more white area you see, the more fat has built up and disrupted healthy liver structure.
In the fructose-only mice — labeled CF in the figure — the liver was filled with these white areas. That’s bad. It means the liver is swollen with fat and starting to break down structurally.
But in the mice that got fructose plus inulin — labeled IF — there was dramatically less white in the liver image. In other words, way less fat.
Just focusing on those two groups (fructose vs fructose+inulin), the message is already clear: adding inulin fiber leads to a substantial reduction in liver fat.
So, in the big picture, fiber improves health. More specifically, in this context, inulin protects the liver from the fatty buildup that fructose normally causes.
How Fiber Changes Liver Metabolism
That result alone is interesting and lines up with a lot of human work suggesting fiber protects metabolic health. But this isn’t even the part that’s most exciting.
The really exciting part is how fiber is doing this.
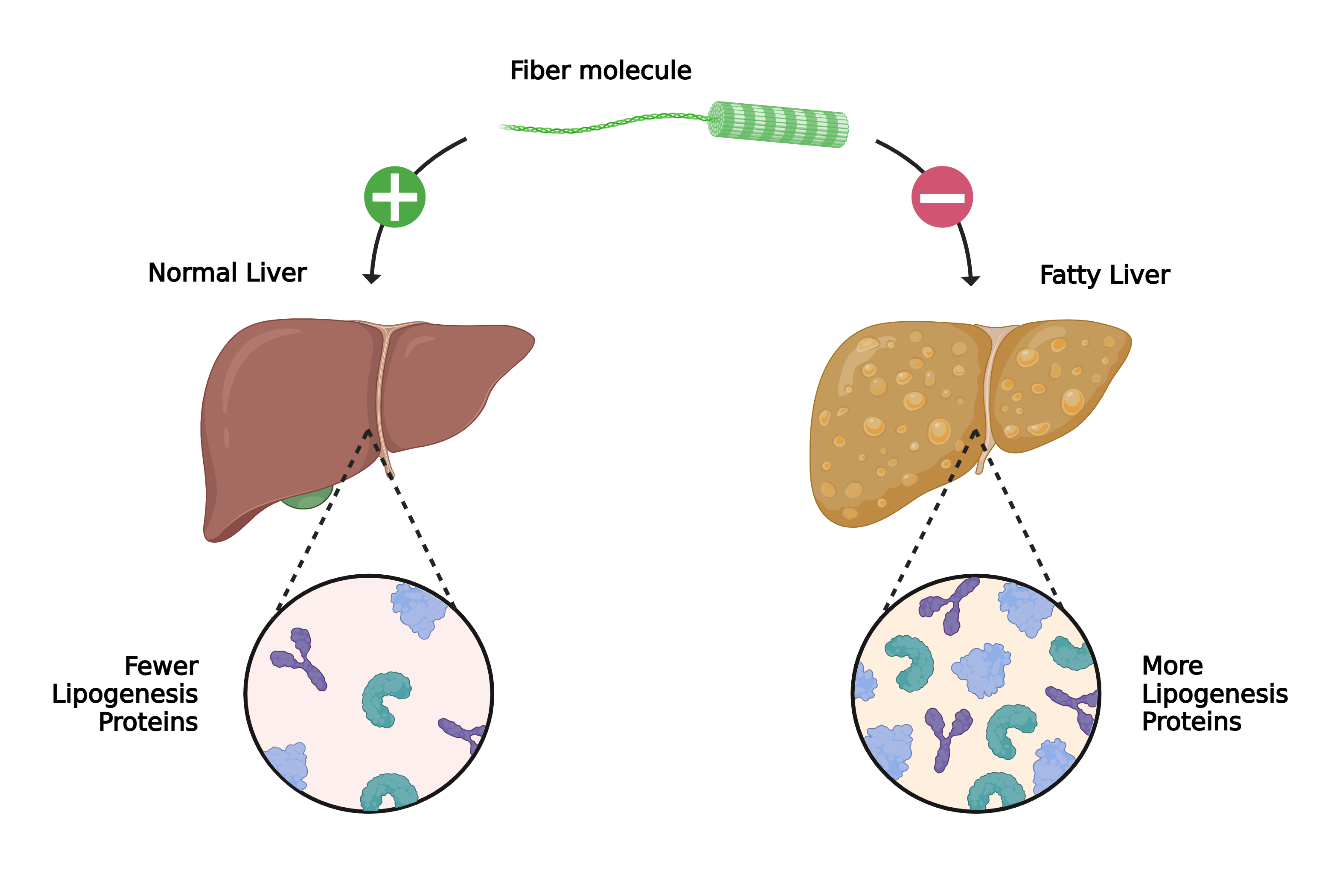
The researchers found that inulin reduces the buildup of fat in the liver by dialing down something called “lipogenesis genes.” Let’s unpack that.
“Lipogenesis” just means “making fat.” Your body can convert excess sugar into fat through a set of enzymes (proteins that accelerate chemical reactions). The genes for those enzymes basically act like blueprints. When those genes are more active, more fat is built.
Inulin lowered the expression of these lipogenesis genes. Plain language: the presence of inulin made the liver less eager to turn fructose into fat.
On top of that, inulin encouraged the liver to break down fat. The study showed that liver cells exposed to fructose plus inulin ramped up metabolism of fat molecules. “Metabolize” here means “burn for energy” instead of “store for later.” So you’re not just blocking the creation of new fat — you’re also helping clear out the fat that already exists.
Put simply:
Less fat being made.
More fat being burned.
That’s a powerful shift.
Inulin converts fructose into a protein we often try to increase in our cells
How much is needed for supplementation?
More on the fructose ‘Spill-Over Effect’
All of that is included in the complete analysis, along with access to a private podcast, live sessions with me, a library of articles and videos, and much more as a Physionic Insider:
The “Fructose Spillover” Problem
There’s another piece, and this one is huge: fructose spillover.
When you eat fructose, it’s supposed to be absorbed and processed in the small intestine first. But with high intake, that system gets overwhelmed. Fructose can “spill over” to places it shouldn’t be.
There are two main spillover problems:
Spillover to the liver: When too much fructose reaches the liver all at once, the liver gets hammered. It starts converting that fructose into fat. That’s one way you get a fatty liver. This can also lead to fibrosis — a stiffening and scarring of the liver as it becomes damaged.
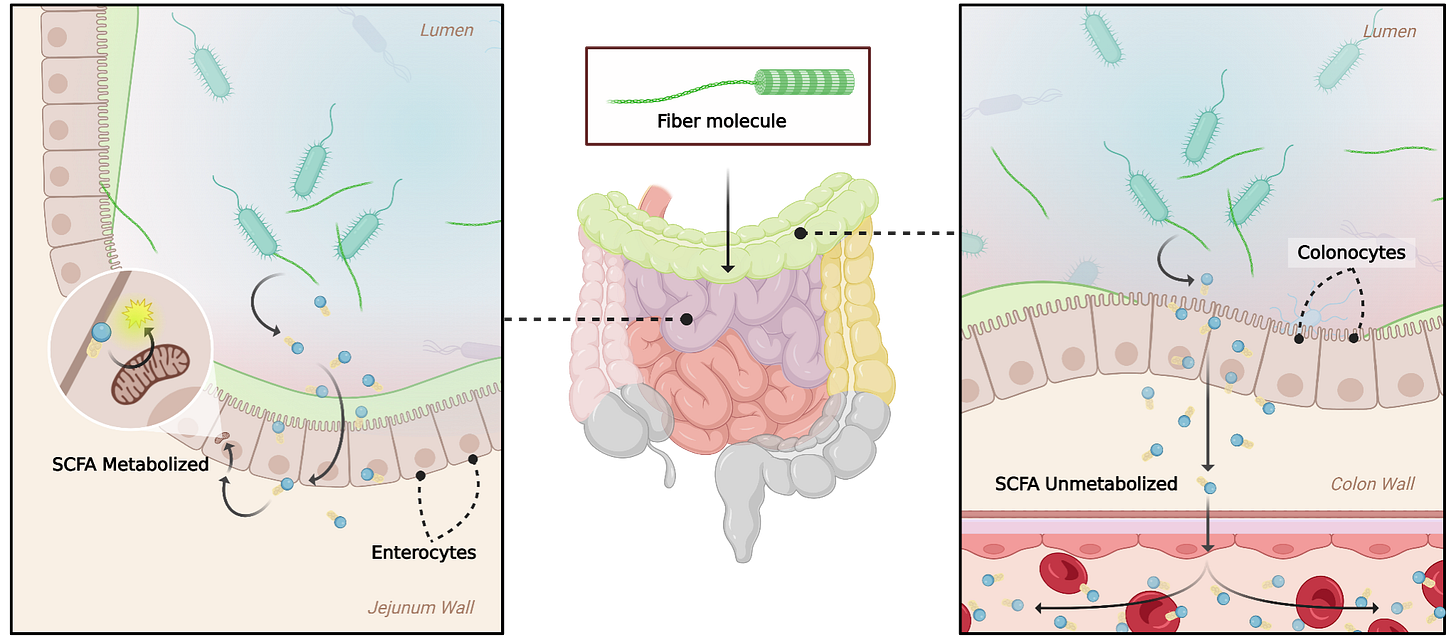
Spillover to the colon: The colon is the last part of the intestine. Fructose is not supposed to be there in meaningful amounts. When fructose ends up in the colon, it can feed the wrong microbes. That can create dysbiosis, which means an unhealthy shift in gut bacteria. Dysbiosis can then generate extra fats that get transported back to the liver, creating even more burden.
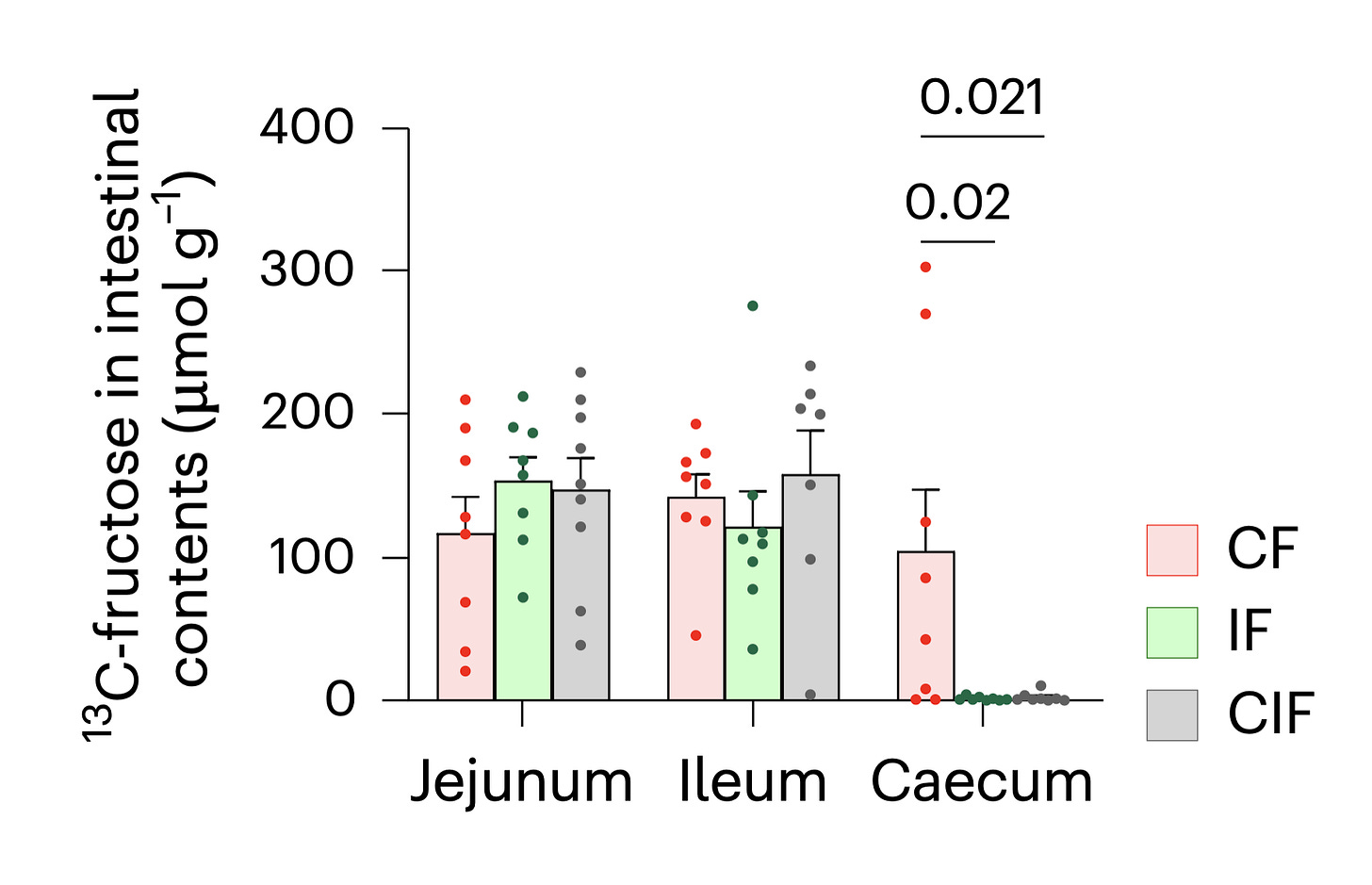
Now here’s the fascinating part. The study actually measured fructose along the length of the intestinal tract. The first two segments shown were parts of the small intestine. The last segment shown was the colon.
In the groups that got fructose plus inulin (IF and CIF in the figure), fructose basically doesn’t make it to the colon.
Read that again: fructose disappears before it hits the colon… when inulin is present.
This means that fiber prevented spillover. Fructose didn’t reach the colon to cause dysbiosis. And it didn’t slam into the liver in the same damaging way.
That’s not just “fiber makes short-chain fats.” That’s a structural re-routing of where fructose goes in your body.
Why This Is Bigger Than “Fiber Makes Short-Chain Fats”
Most of the common story is: “Fiber feeds gut bacteria. Bacteria make short-chain fats. Short-chain fats are healthy.” That’s still true, and it still matters.
But now, we can say more:
Fiber (inulin) reduces the liver’s production of new fat from sugar by lowering lipogenesis genes. In everyday language: less conversion of fructose into stored fat.
Fiber helps the liver metabolize, or burn, fat molecules instead of stockpiling them. So the fat that’s already there is being used up.
Fiber protects against fructose spillover. It stops fructose from flooding the colon, which protects gut balance, and it reduces the overload on the liver.
The big idea here is that fiber isn’t just passively “good for you.” It is actively defending your liver on several fronts at once.
Where Do You Get Inulin?
All of this keeps coming back to inulin.
Inulin is a type of fiber found naturally in certain plants, especially certain roots and bulbs. You can also buy it as a supplement.
Here’s a non-exhaustive list of foods that contain meaningful amounts of inulin:
Chicory root
Jerusalem artichokes
Garlic
Leek
Onion
People sometimes choose supplements, but concentrated inulin can cause gas or GI discomfort for some. If that’s you, spacing out intake instead of taking a huge amount at once can help.
What This Means for Liver Health
All of this points to one central message: inulin, a dietary fiber, improves liver health through multiple mechanisms that all revolve around stopping the liver from becoming a fatty liver.
A “fatty liver,” in medical language, is called a “steatotic liver.” A steatotic liver is when liver cells are bloated with fat droplets. Over time, that can trigger inflammation in the liver, and then fibrosis, which is like scar tissue forming in the organ. That combination — fat + inflammation + fibrosis — is what drives non-alcoholic fatty liver disease forward.
If you already have something like Non-Alcoholic Liver Disease, focusing on inulin-rich foods should be a priority. That means leaning into foods like chicory root, certain roots and bulbs, garlic, leeks, onions, and similar sources.
Could you just “avoid fructose”? You could, and cutting back on sugary drinks high in fructose is a smart move. But here’s the thing: some of the benefits of inulin go beyond just blocking fructose. So if you only remove fructose and never increase fiber, you’d miss out on advantages that come directly from the fiber itself.
Main Points
Fiber has always had a good reputation, but this new work makes that reputation specific and mechanistic. In animals overloaded with fructose, adding inulin — a fermentable fiber — dramatically reduced fat buildup in the liver and improved liver structure. Inulin did this by (1) turning down the genes that turn sugar into fat and (2) encouraging the liver to burn fat instead of hoarding it. It also (3) blocked fructose spillover into the colon, preventing downstream gut damage and reducing the constant fat assault on the liver. Practically, that means inulin-rich foods like chicory root, Jerusalem artichokes, garlic, leeks, and onions are not just “fiber sources,” they are liver-protective tools. If you’re dealing with, or worried about, fatty liver, especially from fructose-heavy eating patterns, prioritizing those foods (or carefully using inulin supplements, if you tolerate them) is a direct, biological way to defend your liver. And while cutting sugary fructose-heavy drinks is smart, some of inulin’s benefits are independent of fructose restriction — so fiber isn’t just damage control, it’s active protection.
Inulin converts fructose into a protein we often try to increase in our cells
How much is needed for supplementation?
More on the fructose ‘Spill-Over Effect’
All of that is included in the complete analysis, along with access to a private podcast, live sessions with me, a library of articles and videos, and much more as a Physionic Insider:
Dr. Nicolas Verhoeven, PhD / Physionic
References
[A] Reynolds A, Mann J, Cummings J, Winter N, Mete E, Te Morenga L. Carbohydrate quality and human health: a series of systematic reviews and meta-analyses. Lancet. 2019;393(10170):434-445. doi:10.1016/S0140-6736(18)31809-9
[B] Threapleton DE, Greenwood DC, Evans CE, et al. Dietary fibre intake and risk of cardiovascular disease: systematic review and meta-analysis. BMJ. 2013;347:f6879. Published 2013 Dec 19. doi:10.1136/bmj.f6879
[C] Whelton SP, Hyre AD, Pedersen B, Yi Y, Whelton PK, He J. Effect of dietary fiber intake on blood pressure: a meta-analysis of randomized, controlled clinical trials. J Hypertens. 2005;23(3):475-481. doi:10.1097/01.hjh.0000160199.51158.cf
[D] Reynolds AN, Akerman AP, Mann J. Dietary fibre and whole grains in diabetes management: Systematic review and meta-analyses. PLoS Med. 2020;17(3):e1003053. Published 2020 Mar 6. doi:10.1371/journal.pmed.1003053
[E] van der Schoot A, Drysdale C, Whelan K, Dimidi E. The Effect of Fiber Supplementation on Chronic Constipation in Adults: An Updated Systematic Review and Meta-Analysis of Randomized Controlled Trials. Am J Clin Nutr. 2022;116(4):953-969. doi:10.1093/ajcn/nqac184
[Study 535] Jung S, Bae H, Song WS, et al. Dietary fibre-adapted gut microbiome clears dietary fructose and reverses hepatic steatosis. Nat Metab. 2025;7(9):1801-1818. doi:10.1038/s42255-025-01356-0.